Ästhetische Kombipakete
– Deine Karriere in der ästhetischen Medizin –
Die Ästhetik-Pakete bieten Dir umfangreiche Informationen zu den Produkten, der Wirkungsweise, den Nebenwirkungen und Komplikationen der Behandlungen. Du erhältst wertvolle Tipps zur Anwendung, Dosierung und Aufklärung der Patienten. Digital stellen wir Dir Skripte, Aufklärungen u.v.m zur Verfügung. Die Pakete sind CME-zertifiziert und nach erfolgreichem Abschluss erhältst Du Deine Zertifikate per Post:
Alle Videolektionen von:
✓ Botulinumtoxin
✓ Hyaluronsäure
✓ 44 Lektionen
✓ 4 CME Punkte
✓ 2 Zertifikate per Post
✓ Fortbildungsskripte (PDF)
✓ Patientenaufklärungen (PDF)
✓ Praxisvideos mit Patienten
✓ Onlinezugang (18 Monate)
1.182€1.284€
Alle Videolektionen von:
✓ Hyaluronsäure
✓ Fadenlifting
✓ 51 Lektionen
✓ 2 CME Punkte
✓ 2 Zertifikate per Post
✓ Fortbildungsskripte (PDF)
✓ Patientenaufklärungen (PDF)
✓ Praxisvideos mit Patienten
✓ Onlinezugang (18 Monate)
1.248€1.424€
Alle Videolektionen von:
✓ Botulinumtoxin
✓ Hyaluronsäure
✓ Fadenlifting
✓ 76 Lektionen
✓ 4 CME Punkte
✓ 3 Zertifikate per Post
✓ Fortbildungsskripte (PDF)
✓ Patientenaufklärungen (PDF)
✓ Praxisvideos mit Patienten
✓ Onlinezugang (18 Monate)
1.842€2.066€
Alle Videolektionen von:
✓ Botulinumtoxin
✓ Hyaluronsäure
✓ Varikosis
✓ Lipolyse
✓ 65 Lektionen
✓ 5 CME Punkte
✓ 4 Zertifikate per Post
✓ Fortbildungsskripte (PDF)
✓ Patientenaufklärungen (PDF)
✓ Praxisvideos mit Patienten
✓ Onlinezugang (18 Monate)
1.962€2.168€
Alle Videolektionen von:
✓Botulinumtoxin
✓ Hyaluronsäure
✓ Fadenlifting
✓ Varikosis
✓ Lipolyse
✓ Needling
✓ 117 Lektionen
✓ 5 CME Punkte
✓ 7 Zertifikate per Post
✓ Fortbildungsskripte (PDF)
✓ Patientenaufklärungen (PDF)
✓ Praxisvideos mit Patienten
✓ Onlinezugang (18 Monate)
2.942€3.332€
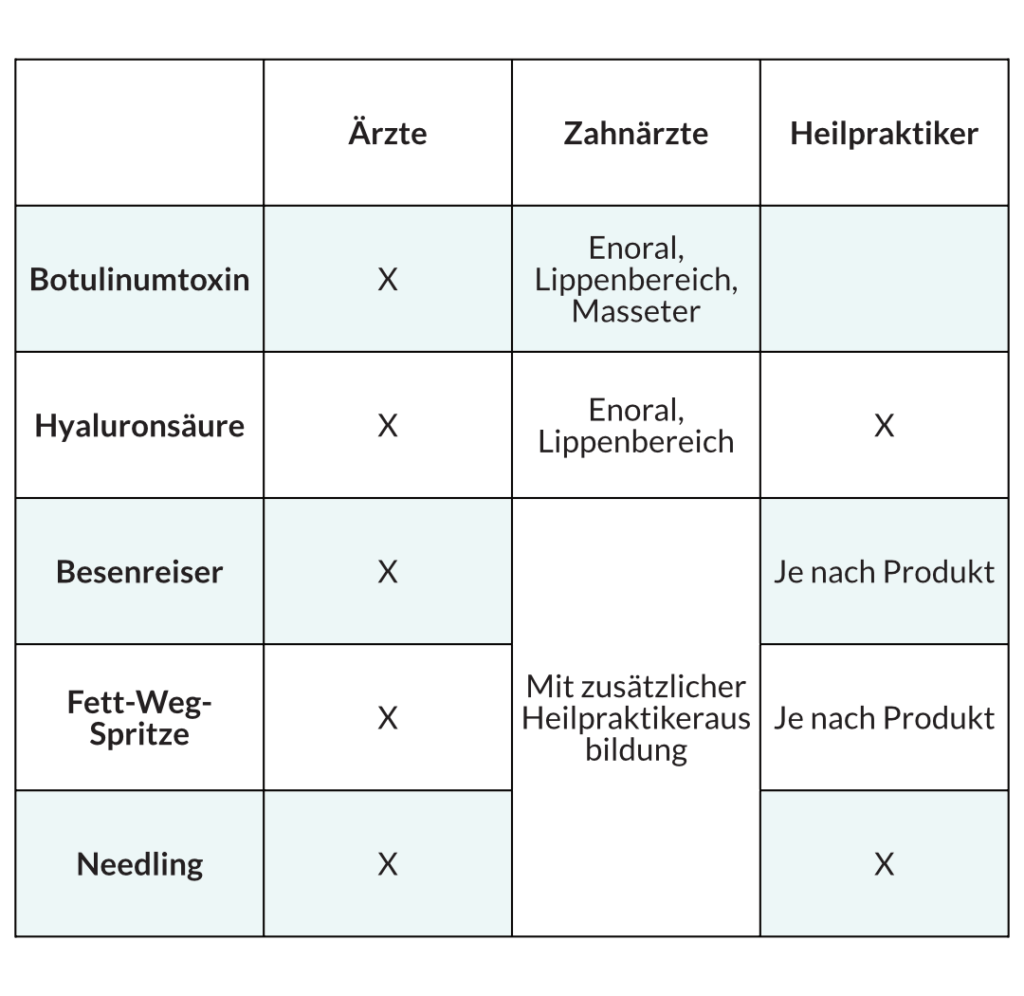
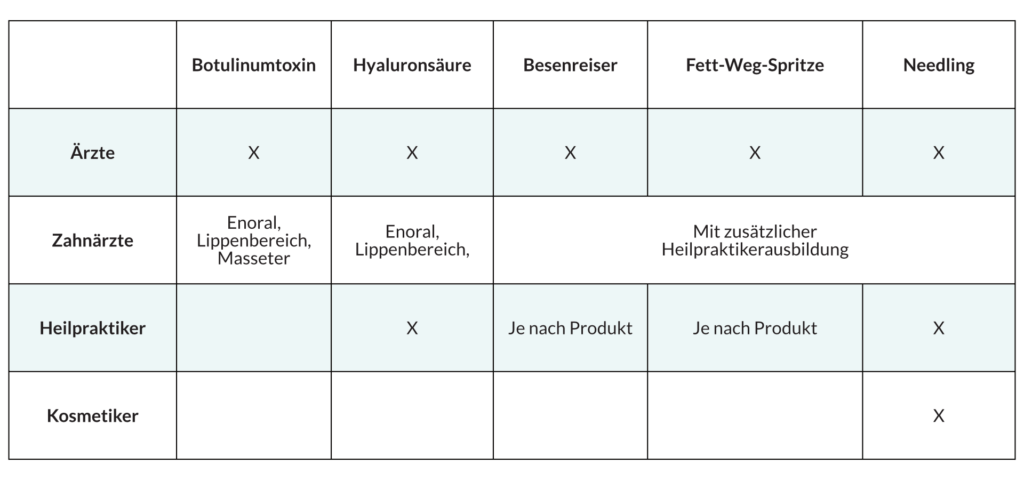
Wer darf was behandeln?
Exklusive Mitgliedschaft in der Ästhetisch Medizinischen Akademie
Eine Investition in Deine berufliche Zukunft: Als MEDILOGIN-Mitglied profitierst Du während und nach Deiner Weiterbildung von vielen Vorteilen!
Vorteile verschiedener ästhetischer Behandlungen
Das Erlernen verschiedener Behandlungen der ästhetischen Medizin wie Botox, Hyaluronsäure, Varikosis und Lipolyse kann viele Vorteile bieten.
Zunächst einmal ermöglicht das Erlernen verschiedener Behandlungen der ästhetischen Medizin einem medizinischen Fachpersonal ein breiteres Spektrum an Kombinationsmöglichkeiten. Insbesondere die Faltentherapie bietet ein hohes Maß an Kombinationsmöglichkeiten an. So können Botulinumtoxin-Behandlungen mit Hyaluronsäure-Injektionen ergänzt werden (z.B. Augenfalten & Tränenrinne). Viele Behandlungen können in einer Sitzung durchgeführt werden und verbessern das Outcome.
Zudem kann das Erlernen verschiedener Behandlungen der ästhetischen Medizin auch dazu beitragen, dass Patienten ein höheres Maß an Vertrauen in ihren Arzt haben. Wichtig dabei ist eine fachlich kompetente Aufklärung und Einschätzung über die Ergebnisse und möglichen Komplikationen. Viele Patienten bleiben bei demselben Behandler, da das Vertrauen in das Ergebnis eine sehr wichtige Rolle spielt.